It pains me to say this, but after more than 5 years of continuous sobriety—5 years in which I lived in rehabs and halfway houses, worked in the drug and alcohol treatment industry, and spent thousands of hours attending 12-step meetings—I have finally come to grips with the fact that I was a woefully incompetent alcoholic and addict. Now, to be clear, this admission does not mean I was not an alcoholic and an addict. It simply points out that I was really badat being an alcoholic and an addict, a development that was greatly influenced by the fact that I sobered up at the ripe old age of 22 and could never seem to get my hands on any drugs or booze during most of my active alcoholism. For example, my parents went away for vacation for a couple of weeks this one summer, leaving my delinquent 20-year old self to watch the house and what I thought would be a generous amount of alcohol therein. Much to my surprise, I discovered when I got to the house that they’d already caught wise to the fact that their son was a lush and locked up all of the hard liquor before they left, with the exception of a few bottles of wine, a 6-pack of Rolling Rock and a half-bottle of cooking brandy. It was less than a week before I was down to my last 4 bottles of beer, having dispatched of the brandy and wine, and needed to be cagey and creative in finding something else around the house to help get me messed up until I could convince someone to go on a booze run for me. Naturally, like millions of other young Americans would do in a similar situation, I went to the medicine cabinet to try and get some little relief.
What I found there was not encouraging. Instead of coming upon a treasure trove of Oxycontin and Percoset and Vicodin, I found a maddening assortment of blood pressure pills, allergy medications and things that wouldn’t get me high in the slightest. So, I was reduced to pulling out every single medication in the cabinet and cross-referencing it with their Wikipedia entries to try and scientifically determine if any of them could get me wasted. The only pill I found that came close to fitting the bill was Amitriptyline, a tricyclic antidepressant medication that my sister took for her migraine headaches. It didn’t look like the sort of drug that would be enjoyably abusable, but Wikipedia listed drowsiness as its number one side effect and the bottle they came in had one of those no drinking symbols on it, so I grabbed a small handful of the things, washed them down with a Rolling Rock and waited on my couch to see what would happen next. Well, I waited for a little while, but my impatience got the better of me and after 15 minutes of nothing spectacular happening, I got up to take a couple more pills and grab another beer from the fridge. The last thing I remember is lying down on the couch, watching that one romantic comedy where Mark Ruffalo plays some sort of ghost architect who’s haunting/wooing Reese Witherspoon in an implausibly nice apartment in downtown San Francisco, wondering why I’m watching that romantic comedy where Ghost Ruffalo macks on Reese Witherspoon and then everything goes black.
When I woke up in my drugged and groggy state, I looked around me and quickly deemed the experiment a success. I was still on the same couch, it was still dark outside and the damn Ruffalo movie was still playing on the TV so I figured I couldn’t have been out that long. Then, as I tried to get up, I noticed that I’d been asleep long enough to drool over about a square foot of couch cushion and that my jeans were soaked with what I could only hope was my urine. Nonplussed, I slid myself off of the couch and crawled over to the side table where my phone was sitting to see how long I’d been out. I figured that it’d be about 10:00 at night and as it turns out I was pretty spot on. The only problem was that it was about 10:00 at night…the next day. So, to recap, in an attempt to get high, I abused an unknown quantity of non-narcotic, tricyclic antidepressants and ended up passing out for 24 hours. Like I said, I was an incompetent addict and alcoholic. I was also a lucky one.
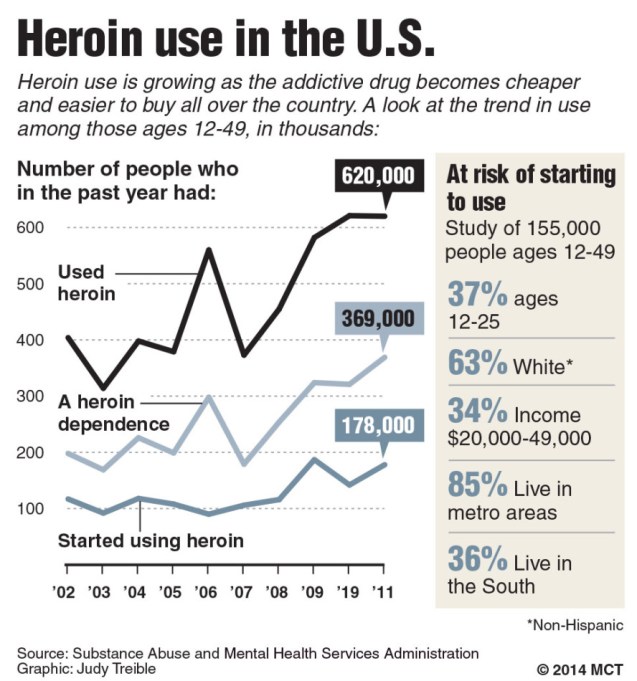
For millions of children and young adults across America, the shelves of their parent’s medicine cabinets are filled with prescription drugs—Vicodin, Percoset, Oxycontin, Opana, Lortab, Dilaudid, methadone, Valium, Xanax, Klonopin, Ativan, Ambien, Adderall, Ritalin, codeine cough syrup, Fentanyl patches—all of them readily available and ripe for the taking. The standard line from the leading lights of the federal anti-drug movement for years had been that marijuana is a “gateway drug” that somehow propels users down some nebulous and slippery slope into the abuse of hard drugs, despite the fact that the vast majority of heavy drug users start abusing licit drugs like alcohol and tobacco before they graduate to weed. However, while there is little evidence to support the theory that marijuana presages some linear progression towards hard drug use, there is more than enough to definitively prove that the abuse of prescription pain relievers and heroin is intimately linked. According to a recent by the Substance Abuse and Mental Health Services Administration, Americans between the ages of 12 and 49 who had abused prescription painkillers were 19 times more likely to have initiated heroin use recently than those who hadn’t and a staggering 4 out 5 new heroin users reported abusing pain pills in the past.
Understandably, this surge in prescription drug abuse over the past decade or so has caused the substance abuse treatment, prevention and recovery communities to revaluate their priorities and double down on their efforts to halt the growth of this epidemic, but there is little that can be done. While it is laudable that the Office of National Drug Control Policy’s Office of Demand Reduction(1) is addressing the problem by raising awareness, championing emergency overdose reversal medications like Naloxone and trying to integrate substance abuse treatment into our mainstream health care system, these actions amount to little more than a band aid on a bullet wound because no one seems to be interested in stopping the production and distribution of billions of abusable prescription medications.
At least, I certainly hope federal government isn’t interested in stopping the production and distribution of these drugs because, if they are, they’ve proven themselves so incompetent that I’m tempted to ask them to pee in a cup for me. You see, the federal government spends around $15 billion every year in an attempt to reduce the supply, sale and use of illegal drugs in America, an amount of money that would seem sufficient to make a dent in the proliferation of prescription drugs, yet has somehow helped to create an environment in which there are enough opioid prescriptions written in this country in a single year to provide every adult American with enough pills to medicate themselves every 4 hours for an entire month. It would seem that while our government was busy spending billions of dollars toincarcerate more than 100,000 men and women in federal prison and filling the coffers of the Department of Homeland Security, they gave short shrift to the prescription drug epidemic developing in their own backyard. The end result is that, in 2011, drug overdoses were the leading cause of injury death in America, resulting in the passing of 41,340 people. Of those 41,340 deaths, a staggering 22,810 of them were related to pharmaceuticals, an amount that eclipsed the number of overdose deaths for all drugs just a decade earlier.
The shape of things to come for prescription drug and opiate addiction may not look good for the nation as a whole, but it looks even worse for places like Cincinnati and Northern Kentucky, where more than a decade of aggressive pill pushing and prescription drug abuse has led to one of the worst heroin problems in the country. With cash-strapped prescription opiate addicts being forced to switch to heroin to maintain their habit, abuse of the drug has skyrocketed over the past 4-5 years, leading to a corresponding rise in heroin related arrests, emergency room visits, court cases and deaths. In Northern Kentucky’s Campbell County, heroin abuse has become so endemic that, at any given time, roughly 50% of inmates in the county jail will be there for heroin-related charges, while things have gotten so bad in Ohio that officials in Butler County are considering a proposal to commandeer a wing of county-owned nursing home and turn it into a detox center. Regardless of which side of the river you’re on, the number of overdose deaths have been rising at a frightening rate, with some county coroners finding themselves unable to provide accurate statistics for how many addicts have died in 2014 because the bodies are coming in so fast that they’re 3 months behind on their toxicology reports.
For me, this sea change in the nature of addiction in Greater Cincinnati came when I moved back in 2013 after spending 2 years in Baltimore getting my Masters in Social Work. In Baltimore, a city that has suffered the unenviable distinction of being the “heroin capital” of America and one in which nearly 1 out of every 10 residents is addicted to the drug, heroin has long been an inescapable fact of life. It was not a surprise when I was working as a case manager at an HIV clinic in West Baltimore to see men and women come in with track marks on their arms or to talk with folks at AA or NA meetings who shot up for decades before getting clean.
In the City of Baltimore, the using patterns for heroin followed the familiar socioeconomic narrative that is well-worn in many of America’s major cities, wherein the poor were far more susceptible to abuse than the middle and upper classes. The heroin epidemic in Baltimore is the product of decades of economic and racial stratification in which wealth and jobs fled from urban areas, leaving a void that has since largely been filled by an underground economy in which the drug trade plays a vital role. When I came home a little over a year ago, I expected Cincinnati’s burgeoning heroin epidemic to resemble Baltimore’s. It did not. Since the locus of Cincinnati’s and Northern Kentucky’s heroin problem lay not with socioeconomic inequities, but with the overprescription of pain pills, the barriers of class and place that have traditionally been at the heart of heroin use in America have been torn down. In Greater Cincinnati it doesn’t matter if you live in the city or the country, if you’re rich or poor, if you’re young or old, or if you’re black or white. All you need is a small prescription drug habit and you’re well on your way to being a full fledged junky.
Having never been addicted to pain pills or heroin, I can’t provide any personal insight as to the cultivation and the horrors of this particular form of addiction. However, residents of a couple sober living houses run by New Foundations Transitional Living were nice enough to invite me into one of their homes a couple of weeks ago and share their experiences with opiate addiction. The stories of the young men I talked to all had their differences—some started younger, some had family members who used, some had done time in prison—but, ultimately, they were all variations on a single theme: the insidiousness of the disease of addiction.
“How’d you first come to start using pills?” I asked Sam, one of the house’s most senior members, as we sat in the dining room of one of their sober living houses in Cincinnati’s Price Hill neighborhood.
“It just kind of happened, you know what I mean?” Sam told me. “It wasn’t like one day I was like…’I’m going to start using pills every day.’ It just happened. First it was the pills and then the pills went to crack and then they were too expensive and then the heroin was cheap.”
At 22 years old, with his easy smile and his short blond hair stiff with product, Sam looks as unassuming and ordinary as any other product of the American middle class. No one—and I mean no one—would take a look at this young man and think that he was an ex-heroin addict who had been arrested for a Felony II burglary 18 months earlier. But that’s what happened. And it all started with the pills.
“I started using pills when I was 16.” Sam told me. “It was just recreational at first, but I knew I liked it way too much, you know what I mean? It really picked up during college because I knew I could do Adderall to stay awake and opiates to come down, and then it started becoming, ‘okay, the opiates are keeping me awake long enough, as long as I don’t do too many of them and then I could just crash. And then, as an alcoholic, I couldn’t do anything about it and it just progressed from there and the pills became too expensive so I went to heroin.”
“Now, switching from the pills to the heroin, how did that work?” I asked. “Did you snort it or start shooting up or what?”
“I never shot heroin, because I never had anyone around to show me how to do it.” he said.“Now, if I had had someone sitting there showing me I guarantee I would have, you know, done it. But I just found it one day and knew I could snort it, and that’s what I did. It didn’t make me any better or any worse.”
As it turned out, Sam’s housemate Catfish never had the same difficulty finding a using role model. Catfish(2) was raised in a family where the chaos of active addiction was always present. A cherub cheeked, rail-thin redhead who looks like he’s 21 going on 16, Catfish is the little brother of the house and, arguably, the resident who needs the most support. Like Sam, Catfish got started by abusing pills, but, unlike Sam, he did so at a startlingly young age.
“I was the first kid out of all those kids who started drinking and doing that stuff” Kyle told me. “I mean I started drinking when I was 9 years old, that’s when I took my first swig of alcohol, but I wasn’t drinking every day. I remember, when I was 10 years old I got introduced to Adderall, Xanax…I got introduced to the pills first.”
“Wow…10 years old…so you were in 4th grade when you started doing pills?” I asked.
“4th grade, yeah…yeah…still in elementary school…and my thing for a while was like, I got introduced to Adderall first and I was doing that until I got introduced to weed and then I started mainly doing that…”
“Were you prescribed Adderall?” I asked.
“No,” he said. “My friends had it…I mean, that’s how I got introduced to it, cause, like, most the kids I went to school with was on Adderall and when they introduced it to me, I mean, I took it. Like, I remember I went to this girl’s house and she had Adderall, her mom had Xanax and it was all just up there in the cabinet…sitting there in the cabinet…and she gave me a handful. I went home that day, first thing I did was the Adderall, stayed up on it. And then the next day I still had the Xanax, I didn’t take ’em, and she told me—I mean, I could not sleep at all. I went to school, my friends saw me and were all like, ‘what the fuck?’ and she told me, she said, ‘take some of these Xanax, you’ll calm down.’ So I took the Xanax and calmed down…and it’s been like that every day since…”
“And you were 10?”
“10 years old, yep, and then I got introduced to weed and I fell in love with it.” Catfish said.“That’s all I did was smoke weed…then I started drinking and smoking weed and, I’ll do anything you put in front of me, pretty much. You know what I mean? Next thing you know I’m taking Oxy and snorting Percs. And then I started doing heroin when I turned 18. And my sister introduced it to me—her and her friend—because I remember, I just got a job. Just got a job. And, you know, I just needed something—I was trying to find Percosets—so I could go to work with some energy and feel good because I just started and I was tired…I just remember I kept calling her so I could get some, next thing I know she was driving up to my house with her and her friend and they was blowed. Like their eyes were so red. And, I was like, damn man…I want to feel like that. So I went to the car and she was like, ‘hey, don’t tell anyone, but we did some heroin. You want some?’ And I was like, ‘nah, I’m cool.’ Because I had heard about it and I knew my dad was on it, so I knew…I had sort an idea of what people said about it. You know what I mean? And then, they tell me, ‘it’s just like Percosets, but it’s cheaper. It’s just like doing a Perc. And I was like, ‘it can’t be that bad” cause I do Percs all the time and it’s just like a Perc. So, I did some heroin and…6 months later I’m homeless. My mom’s hooked on it. My brother’s hooked on heroin. Both my sisters hooked on heroin. Sleeping in the woods. It took off that quick too. I remember 2 weeks after I started snorting heroin, I started shooting it.”
“2 weeks?” I asked
“2 weeks out there, yeah.” he told me.
“You said something earlier about your family sleeping in the woods?”
“Yeah, they all do except for my brother, but that’s cause he lives over in the house with me. My mom, my little sister, my older sister…they’re all sleeping in the woods over here on Glenway [ave.]” Catfish said. “I see my mom every once in a while, but she’s real real strung out and and so’s my sisters, so I can’t be around ’em much.”
“Is your dad still in the picture?” I asked.
“My dad? He’s been in and out prison for meth—for making meth and stuff—like I haven’t seen him in 2 years.” Catfish told me. “I talked to him yesterday, though. Somehow he got my number and I talked to him and I asked him how he’s been, because he’s strung out real bad, you know, he’s been like that most of my life. But, soon as I ask him how he’s been, he’s like, ‘well, I haven’t been in prison in over a year, or jail, got my meth lab going back up.’ So, I’m like, ‘yeah, dad. It doesn’t sound like you’re doin’ too good.’ Like, he’s telling me all of this stuff like how he got this huge hole in my arm because he shot some meth and it missed and it ate a huge hole in his arm and he almost died. Told me that the doctors told him that if he’d laid on the couch one more day he’d be dead. He said he was in the hospital for 2 days. He was supposed to be there for 2 weeks, but he couldn’t get no heroin so he left the hospital…said he left a couple of days ago.”
With that, Catfish stopped for a moment and looked around the room.
“This is my family right here.” he said, pointing at his housemates. “This is who I wake up to every day, this is who I talk to every day. This is, this is…all I have. I mean, I don’t go to Thanksgiving, Christmas with my family because I don’t see them, I don’t talk to them, I don’t know where they are. You know what I mean? So this is what I have. This is what I wake up to right here.”
“That’s a good thought there Catfish.” said Jason, a resident who lived at another of New Foundation’s houses. “It’s like a family unity thing for me. You know, I love everybody at my house. I call it my home and I can’t wait to get there sometimes. It’s a better network than being out there on the streets with the dope fiends and the junkies and all of that, you know what I mean? It ain’t no good out there. These guys here—all these guys right here—I live with them and I love all of them, you know what I mean? They care about you. When I was out there in the streets ain’t nobody care for you…they just want what you got or your dope money, whatever…whatever you can offer to them, and then they’re done with you. These guys are there for me when I’m up and when I’m down.”
“Well, considering y’all are so close, how hard is it when somebody you’ve lived with for a while, you know, goes back out?” I asked.
“Hard…hard…man, it’s really hard.” Jason said as everyone else nodded their heads and murmured in agreement.
“These guys took me everywhere they went when I got here.” Catfish said. “I was able to learn from ’em. I was able to grow with ’em, so, it’s hard, you know what I mean, to see one of ’em go back out, cause that’s your family. The whole time I was out there using and stuff, it was like I had no feelings. I wasn’t able to feel that love and trust and all that, you know what I mean? And like, since I’ve been sober, I feel that at the house, I feel that love and stuff, so now when I go back out I feel the pain from it. Like, before, if I was high or something, when I was using…when my family members die—stuff like that, it didn’t really effect me because I had all the drugs and stuff. I couldn’t feel it. It was hard to cry. It was hard to feel that loss. But now I’m sober, and I’ve been with these guys so long that when go back out and start using again, you know, it hits you.”
Everything was quiet for a while after that, until Joey—the oldest in age at 30, but the newest in the house, having only been there for 3 weeks—spoke up:
“That heroin man…” Joey said, to no one in particular. “I had an abscess on my back.”
“On your back?” I asked.
“Yeah, bruh.” Joey said, as he stood up from his chair and lifted up his shirt to expose a thin scar running down his spine. “Went through my bloodstream and sat on my back. The guys here don’t know about it. I ain’t even tell nobody about it. I was paralyzed for 8 and ½ months. In Drake Hospital, had to go through rehabilitation. Learn how to walk and all that shit. And then get out and shoot dope again.”
“And how long was it between the time you got out of Drake and the time you started shooting up again?” I asked.
“Uhhh, when I got out they gave me Perc 30s…the time release morphines…I had ’em. But I’m selling ’em. They day I get out I’m selling ’em…selling ’em to get heroin, bruh.” Joey told me. “Yeah, I was thinking, while I was selling ’em, that if this ain’t gonna stop me from using, you know, being paralyzed and cooped up in a bed, then what the fuck is?”
No one said anything. No one said anything, not because we were shocked by Joey’s behavior—which was little more than a stark demonstration of the insanity of active addiction—but because we couldn’t answer his question. At least I couldn’t answer it. I have gone through the hell of active addiction; I have spent the bulk of my adult life in recovery; I have worked in therapeutic capacities with addicts and I have written policy papers on issues concerning addictions, and still—after all of that—I am no closer to understanding why one addict gets clean and another doesn’t then I was when I started. And that’s the problem. I fully understand why it is that people become addicts. I understand that there is a definite hereditary component to addiction and that the environment in which a person is raised—their socioeconomic status, their family life, their geography—has a profound effect on their chances of becoming an addict. I know that the overprescription of opioids and benzodiazepines is the driving force behind an unprecedented epidemic of prescription overdose deaths. What I don’t know is how to put a stop to a pharmaceutical-industrial complex that has made billions of dollars off of the suffering of others and which still continues to market newer, deadlier versions of the drugs that have already killed so many. I don’t know why it is that some addicts get clean and others don’t; why some are chronic relapsers and others get it in their first time around. And I don’t know how many of the men I spoke with at New Foundations are going to be clean a year from now and, if they aren’t clean a year from now, how many of them will be alive. I can’t tell you that about them and I can’t even tell you that about me. Drugs, like the pharmaceutical giants and cartels that sell them, don’t care how much clean time someone has. All they care about is getting you high and maybe, just maybe, getting you dead.
——————
(1) In the interest of full disclosure, I must mention that I was an intern with ONDCP’s Office of Demand Reduction in 2012-13. I would say that I was unpaid, but that would be untrue as I was given 2 boxes of special Presidential M&M’s from the White House Easter Egg Roll as compensation.
(2) Catfish’s real name is actually Kyle, but since there was already another Kyle living in the house when he got there, they took to calling him Catfish to avoid confusion.
Categories: Drug News

There are no words . . .
Blessings,
Anni
Anni Macht Gibson (513) 448-6511 gracefullsunangel@gmail.com
Sent from my iPhone
>
Absolutely amazing writing. Absolutely terrifying truths about the PIC and it’s heartless, inhumane tactics of financial gain with the blood of people like myself. I too have shot up heroin for many years. The story in this post echoes mirror images of despair and pain from the past. If you ever need someone to aid one of your IV heroin/cocaine related topics, I would love to share some of my past. Not sure how you found me but this post really hit home for me. Thank you.
Dustin J.
My blog site is http://www.jdusty45.wordpress.com
Thanks again
Drew, I have so much to say and I have nothing to say. All I know for sure is that true Love, received, changes everything. So I keep giving Love and receiving Love and create a better world. Excellent as always. Thank you for sharing this side of you. L.
A fantastic article. In partial response, I wish to share an op-ed from several months ago related to the issue of opiate/heroin addiction. I have written the novel “Addiction on Trial” as a way to reach a wider audience of readers and educate through the back door using fiction, but based on medical and legal truths. If we educate, then we can effect change – as a physician author, I hope my blog and book will help. http://www.addictionontrial.com
SOLUTIONS TO THE HEROIN & OPIATE EPIDEMIC
March 27, 2014 • skassels • 1 Comment
“The Scourge of Heroin Addiction”
Op-ed published by the Boston Globe April 1, 2014 http://b.globe.com/1kAzt54
Governor Deval Patrick has appropriately declared the opioid addiction epidemic as a public health emergency. The governor’s directives will save lives and help to put some brakes on this run away scourge to society. But questions remain and more issues need to be addressed.
For example, why is medication management for the treatment of heroin/opioid addiction scorned by so many? In a recent Boston Globe article, “Heroin Epidemic Exposes Deficiencies In Care System” (http://b.globe.com/1iNFmzo), Ms. Jacobs, Director of Substance Abuse Services for the Commonwealth of Massachusetts, acknowledged, “medications are not used as much as they could be for opiate addictions because of stigmas attached to them, she said.” We watch endless commercials about how to treat illnesses such as urinary incontinence or erectile dysfunction but public service announcements addressing the heroin/opioid epidemic and the proven benefits of outpatient cost effective medication management have been relatively sparse. The governor’s directives, which include public health advisories to educate the public about opioid addiction treatment options, will hopefully demystify common misperceptions, such as crime increases when there is a treatment center in one’s community. In fact, there is a 50% to 80% reduction in crime by heroin addicts when in treatment. (http://bit.ly/OVVRfh ; http://1.usa.gov/1dtb42B)
We read about the blame for the heroin epidemic, but rarely do we address a complex underlying issue – that we as Americans want instant results and we want total pain relief after an injury or procedure. Injudicious prescribing of pain medications undeniably contributes to the problem, and holding doctors accountable is essential; but this is not the only reason we have an unabated heroin epidemic. Other factors include: the war in Afghanistan, which directly led to a surge in heroin production; the reconstitution of oxycontin pills, so they could not as easily be used to “shoot up” or “snort”, resulting in more persons turning to heroin as a drug of choice; the increased availability of opiates through the internet; inadequate mental health treatment services resulting in some patients “self-medicating”; and the lack of addiction treatment facilities due to a common community approach of NIMBY (Not In My Back Yard) along with the stigma associated with seeking treatment for the disease of addiction. Despite the arrest of kingpins and drug pushers, big and small, we still have a supply and demand problem. The supply of heroin has increased and cost is down to as little as $4/bag. As fast as we take drug pushers off the streets, they are replaced by others – there is too much money involved. Governor Patrick is right to focus on the demand side of the issue.
If outpatient treatment is not more widely accepted and available, inappropriate hospitalizations and incarcerations of patients will continue. It is time for our locally elected officials to openly support establishing treatment centers in their communities? We all know heroin addicts, albeit we may not know who they are. They could be any one of a number of patients I have treated: your plumber; the mailman; your kid’s college professor; the IRS agent who audited your tax return; the person selling flowers at the corner; the principal of an elementary school (http://bit.ly/1m6XMbL); someone who works in a mayor’s office (http://bo.st/1hbtN20); or a neighbor; or a family member.
A recent study has shown that less than 20% of individuals needing addiction treatment actually received treatment (http://1.usa.gov/1hYRzvX).. Another study found that only 1 in 10 people with addiction involving alcohol or drugs other than nicotine receive any form of treatment and that “most medical professionals who should be providing addiction treatment are not sufficiently trained to diagnose or treat the disease, and most of those providing addiction care are not medical professionals and are not equipped with the knowledge” (http://bit.ly/1o2l3Ax). Are we willing to accept as status quo the present system of unnecessarily hospitalizing or incarcerating patients? We are wasting tax dollars: it costs up to $50,000 or more per year to incarcerate (http://bit.ly/1iBKSlg ; http://nyti.ms/NW5dGQ) and approximately $5,000 per year for outpatient treatment (http://bit.ly/1rCh3G6). “There are things besides beds that are effective in this system,” Jacobs said. “More people should see this treatment as a viable option.” (http://b.globe.com/1iNFmzo)
There should be just as many public service announcements about addiction as there are Viagra and Cialis commercials. In addition, expansion of addiction treatment services in jails would help to mitigate much of the revolving door phenomenon. Furthermore, we should demand that our medical schools and hospitals improve addiction training of our physicians. While there is plenty of blame to go around, let’s focus on the solutions. The scourge of addiction is in all of our yards. The solution is to decrease the demand with bold public initiatives and a change in attitude. It is both the humanitarian and fiscally responsible thing to do.
Steven Kassels, MD has been Board Certified in Addiction Medicine and Emergency Medicine. He currently serves as Medical Director of Community Substance Abuse Centers and has authored the book, “Addiction on Trial: Tragedy in Downeast Maine”.
Reblogged this on crazy dumbsaint of the mind and commented:
“The standard line from the leading lights of the federal anti-drug movement for years had been that marijuana is a “gateway drug” that somehow propels users down some nebulous and slippery slope into the abuse of hard drugs, despite the fact that the vast majority of heavy drug users start abusing licit drugs like alcohol and tobacco before they graduate to weed. However, while there is little evidence to support the theory that marijuana presages some linear progression towards hard drug use, there is more than enough to definitively prove that the abuse of prescription pain relievers and heroin is intimately linked. According to a recent by the Substance Abuse and Mental Health Services Administration, Americans between the ages of 12 and 49 who had abused prescription painkillers were 19 times more likely to have initiated heroin use recently than those who hadn’t and a staggering 4 out 5 new heroin users reported abusing pain pills in the past.”
Here’s a testimonial of one of the teens we treated at our teen rehab to get a real feel for what it is like to overcome opiate addiction. http://www.inspirationsyouth.com/blog/page/8/
Reblogged this on shawnalcock87's Blog and commented:
This is a great read, I suggest anyone who’s dealt with addiction in they’re lives please take a few minutes and read this!